World Diabetes Day is upon us. Depending on the type and severity of this autoimmune disease, having it can make life infinitely harder: you have to depend on diabetes aids and tools just so that you can survive another day.
As of now, there has been no cure found to treat diabetes but there have been multiple advancements to help people manage the consequences of this autoimmune disease. So on World Diabetes Day DutchReview is going to take the opportunity to raise awareness about this life-threatening disease and diabetes care in the Netherlands. If you’re living in the Netherlands with diabetes, know that you are in good hands.
By Ailish Lalor and Kavana Desai
What is diabetes?
Before we dive into diabetes care in the Netherlands, first let us explain what exactly this autoimmune disease is.
A person is said to have diabetes when the glucose level in their blood is too high. Glucose is a simple sugar that is the most common type of simple sugars that can be found in a lot of vegetables, fruits, and a few grains. When eaten, insulin, a hormone that is secreted in your pancreas, makes sure that this glucose is taken from the bloodstream and sent to the cells for energy.
If this hormone is not being secreted or used well enough, the glucose stays in the bloodstream. If glucose remains in your blood for a long time, it will lead to severe health problems. You might call it a case of a “sugar-rush” but it is far more serious than that.
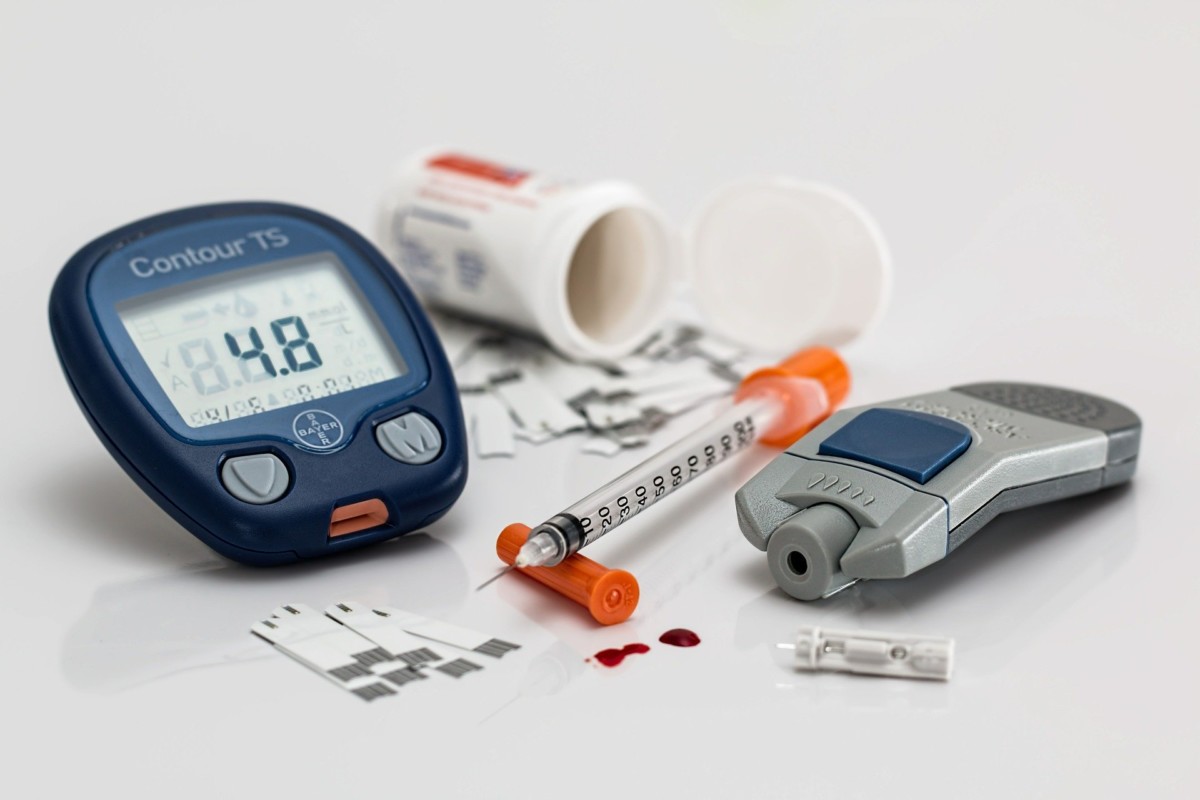
Types of diabetes
Having diabetes means it would be a matter of life and death which makes you more susceptible to cardiovascular diseases, strokes, depression, kidney damage, skin conditions and more. There are several types of diabetes but the most common types are type 1 and type 2 diabetes. However, there are many other forms of diabetes that are often not mentioned in the public discourse. There is growing evidence that both type 1 and type 2 diabetes are autoimmune diseases, even though type 2 has been commonly understood as a metabolic disorder in the past.
The other forms include gestational diabetes (diagnosed only in pregnant women), monogenic diabetes (a genetic form of diabetes), MODY (Maturity Onset Diabetes of the Young, a type 2 form starting at a young age), LADA (Latent Auto-Immune Diabetes in Adults, a form of type 1 diabetes that looks like type 2 because of the gradual development of the disease), Neonatal Diabetes (form of type 1 occurring in the first 6 months of a child’s life, which needs a different form of treatment), MIDD (Maternally Inherited Diabetes and Deafness, which is caused by genetic material transferred by the mother and occurs between 30 and 50 years of age), and cystic fibrosis-related diabetes (which has elements from both type 1 and type 2 diabetes). As you can probably imagine from this list, it can be difficult for different forms of diabetes to be diagnosed correctly.
For anyone diagnosed with diabetes, life changes pretty dramatically. You have to do and eat different things each day: this is hard enough for an average person, but it makes this particularly difficult for the parents of children with diabetes. Diabetics will try to keep their blood sugar steady throughout the day, but this is pretty impossible task, with complications lurking around every corner. Plus, having an autoimmune disease makes you more susceptible to other types of autoimmune diseases such as thyroid disorders. This is known as comorbidity.
Type 1 diabetes
Your immune system is there to protect and kill viruses, bacteria and other disease-causing cells that might find their way into your body. But what do you do when it starts attacking the cells in your pancreas that produce insulin? In that case, your body does not make any insulin at all, and the blood glucose levels would sky-rocket.
People who have this type of diabetes may not be able to eat certain types of food and will have to take insulin every day in order to survive. It is usually diagnosed in children and young adults but can also occur at any later stage. People who have diabetes have to make an estimated 180 extra decisions each day: balancing everything you do and eat every day is complicated. But the consequences of not doing so are severe: they include ketoacidoses and death.
Type 2 diabetes
This is the most common type of diabetes diagnosed in the general population. While in type 1 diabetes, the body does not produce any insulin at all, people with type 2 diabetes do not use the hormone sufficiently. So it is still produced but the body becomes “insulin resistant”. Researchers and doctors are unsure as to why some people develop this resistance, but most research alludes to lifestyle factors like smoking, unhealthy diets, obesity, and a sedentary lifestyle. It can occur at any age and is most often recorded in older adults.
What are the symptoms of diabetes?
According to the Mayo Clinic, the symptoms for diabetes are:
- You feel thirsty all the time
- You have lost an abnormal amount of weight in a short period of time
- You can get irritated easily or have bad mood swings
- Your wounds don’t heal quickly
- You have to pee all the time
- You feel like you haven’t eaten at all even though you had food
- You have fatigue
- You get a lot of infections around your gums, skin or genitals
- You have ketones in your urine
- And of course, a high blood sugar level
If you want to know the cause or prevention of diabetes check here or consult your doctor. Try leading an active life, keeping your blood pressure and blood sugar in check, and be on the lookout for symptoms.
How common is diabetes in the Netherlands?
The Dutch seem to be very proactive when it comes to dealing with diabetes. Diabetes care in the Netherlands is one of the best in the world. According to the World Health Oragnisation’s 2016 Health profile of the Netherlands, the number of deaths caused by diabetes in the Netherlands accounted for only 2%, a little over 6% of the population diagnosed with this autoimmune disease.
The European Commission also measured how much of the population is living with risk factors for diabetes: nearly 60% of the Netherlands is overweight, and nearly 18% are living a very inactive life. Obesity has steadily increased with 10% of the population living with it in 2000 to 13% in 2014 and 22% in 2016.
To fight these underlying risk factors, the Netherlands rolled out some national health programs. One of them is called the National Prevention Agreement which was ratified in 2018. It sets out ambitious goals to make the Netherlands healthier by 2040 but it was revealed in March 2019 that they are still far from reach.
Diabetes care in the Netherlands: does basic Dutch health insurance cover diabetes care?
In short, yes. You are covered for your diabetes care in the Netherlands through your basic Dutch health insurance. However, this comes under your own-risk fee or the deductibles. This means that you have to pay for a part of the medical care and medicines (according to what you set the deductible as) and the rest will be covered. Then you will be reimbursed for your visits to the specialist and for your diabetes aids.
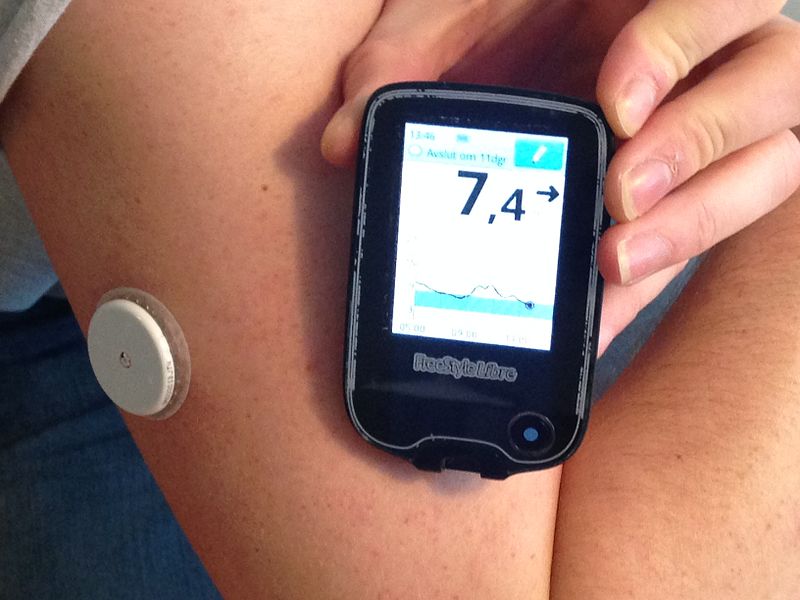
However, there are still significant problems with diabetes healthcare in the Netherlands. One of the major issues is that flash glucose monitors (FSL) and sensors (that is, continuous glucose monitoring sensors (CGM)) are only covered by insurance if you’re under 18, have severe high glucose levels or are pregnant. Both scientific research and diabetics themselves state that quality of life significantly improves with the use of a glucose monitoring system, thus preventing complications later on in life. Most people prefer a glucose monitoring system to a minimum of four finger pricks per day (that is the standard amount of tools for finger pricks covered by health insurance), because you can treat your glucose levels all day instead of a couple of times a day and have no overview whatsoever.
There were changes made to this in November 2019, but the effect was only that children who had grown up using FSL would not have to return the monitors when they turned 18: their insurance would continue to cover the costs of the machine. But for adults with diabetes, the FSL system is still mostly out of reach due to the high costs when it is not covered by insurance. There is a petition with 51,000 signatures to change this, and have FSL and CGM covered by Dutch health insurance.
You are eligible only if your physician prescribes insulin as a treatment method. Don’t forget that referral letter from your GP and do check with your health insurance provider. Make sure to read that fine print with a magnifying glass to know exactly under what conditions this will be reimbursed.
Diabetes care in the Netherlands: getting insulin if you don’t have basic Dutch health insurance
The scenario might always happen: you’re travelling through the Netherlands, and your insulin pens have run out. Or there has been some sort of delay with arranging your basic Dutch health insurance. You’re stuck and panicking because you may need these to live another day.
Don’t worry because there’s a solution to this problem. Everyone living and working in the Netherlands is obliged to have basic Dutch health insurance. If there’s a delay in applying for it, your insurance will be backdated to the date that you arrived here. So if you go out and get a prescription from your GP to go buy your diabetes aids while you are uninsured, they will be reimbursed nonetheless.
However, you will have to pay for this upfront: according to this blog post written in 2015 on Diabetes Sisters, the person paid 27 euros for a visit at the GP and 66.87 euros for five pens. It would have cost her 121.46 euros for 10 pens. However, these costs may vary from provider to provider. So even if you are travelling through, or if you are waiting to apply for your insurance, be sure to have the cash handy.
Are you living in the Netherlands with diabetes? What has your experience been like? Let us know in the comments below!
Editor’s note: DutchReview would also like to thank Danielle De Wit for all of her helpful insights and comments about diabetes care in the Netherlands. We couldn’t have done it without ya!
Feature Image: Steve Buissinne/Pixabay
Editor’s Note: This article was originally published in November 2019, and was fully updated in November 2020 for your reading pleasure.
I believe you are incorrect about the CGM policy. It was changed for 2020. My son (18+) has been using it and he didn’t qualify previously